With an ever-evolving healthcare system, certified medical billing and coding professionals have to stay on top of changing codes, practices, and regulations. Telehealth Services Coding, CPT Evaluation and Management Code and Guideline Changes for 2021, and Opioid Use Disorder Coding provide you with three opportunities to earn continuing education credits, showing your commitment to your healthcare career and patient care.
 Telehealth Services Coding
Telehealth Services Coding
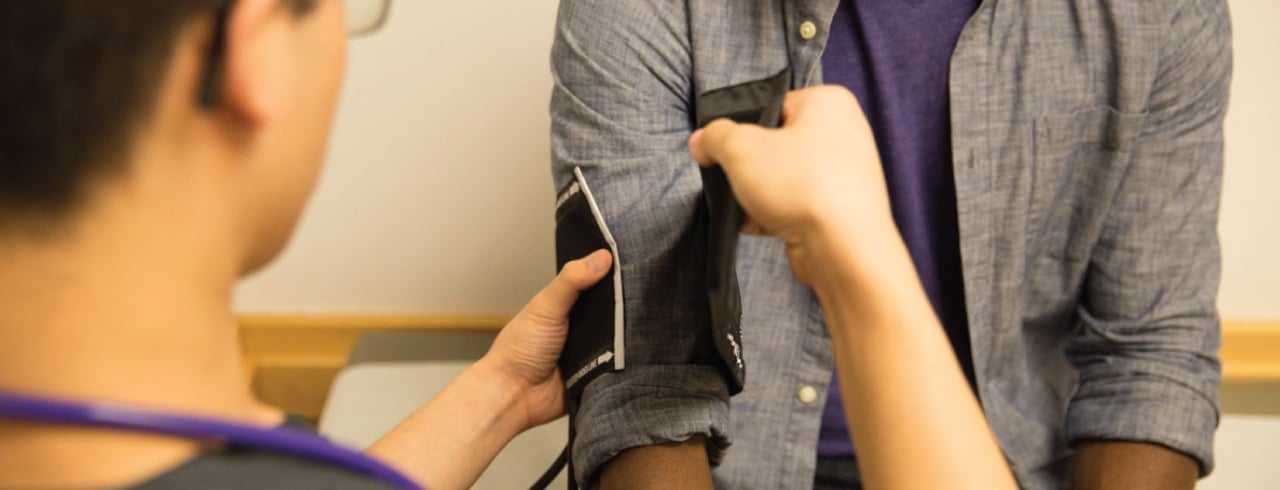
Telehealth services offer the convenience of providing remote healthcare services via telecommunications using a variety of electronic devices. Implementing telemedicine is an important contribution to providing accessible quality health care and preventive services to patients while controlling or reducing costs associated with treating patients and preventing unnecessary emergency services and hospitalizations.
There are now over 100 service codes that can be performed using telemedicine to meet patients' health and wellness needs. Thanks in part to the relaxed regulation triggered by the COVID-19 pandemic, the spike in telemedicine occurrences will continue.
The opportunity to provide health care services via telecommunications using a variety of electronic devices brings new concepts and new terminology, including terms relevant to eligibility and billing for telemedicine services. Through Telehealth Services Coding, you will learn new concepts and new terminology and terms pertinent to eligibility and billing for telemedicine services, including:
- The intent and use of telemedicine services as a benefit to both patients and healthcare professionals, improving access to healthcare for patients with mobility issues, patients who live in rural areas, or those without the resources to travel to their clinic or healthcare organization.
- Types of patient services performed using telemedicine codes
- Types of codes (HCPCS and CPT) used by third-party payers
- Modifiers used for telehealth services
- Benefits of using telemedicine to improve access and outcomes of patients
 CPT Evaluation and Management Code and Guideline Changes for 2021
CPT Evaluation and Management Code and Guideline Changes for 2021
According to CMS’s Comprehensive Error Rate Testing (CERT) program findings for 2019, more than 25% of new and established patient office visits included an error that caused improper payment. Errors include insufficient documentation and incorrect coding.
Improper coding and insufficient documentation of EM (and other CPT) codes result in both overpayments and underpayments. Neither is desirable for accurate documentation, reporting or accounting purposes, and both can subject an organization to unwanted scrutiny from third-party payers.
The 2021 EM coding guidelines for office and other outpatient services are intended to reduce the time and effort spent documenting for office visits or other outpatient visits. They will also reduce the historically high EM error rate because the new guidelines provide healthcare professionals with an intuitive approach to assigning a code.
These significant changes mean the guidelines have not merely been modified; they have been completely rewritten.
The new guidelines for office and other outpatient evaluation and management codes (99202-99215) will improve the accuracy of code assignments and reduce professionals’ time spent on documentation. These codes no longer include key components in their descriptors, and code selection will be based on an improved medical decision-making chart or a defined time range. For example, key components, history and examination, and their elements (history of present illness, review of systems and past medical, family and social history) no longer apply to leveling or selecting an office and other outpatient code. Selection is now based solely on time or medical decision making.
Staying current with annual coding updates is a best practice for ensuring correct documentation, coding, reporting, and billing. Every year updated coding manuals contain new codes for conditions and diseases, new technology, surgical approaches and evaluation, and management services that characterize contemporary approaches to patient care. Through PT Evaluation and Management Code and Guideline Changes for 2021, you will be able to:
- Describe the intent and use of the new EM guidelines
- Define the coding significance of the history and examination components
- Summarize the criteria for choosing an office or other outpatient evaluation and management code
- Recognize the importance of staying current with evaluation and management codes for documentation and coding purposes
- A knowledge of new EM guidelines to office and other outpatient encounters
 Opioid Use Disorder Coding
Opioid Use Disorder Coding
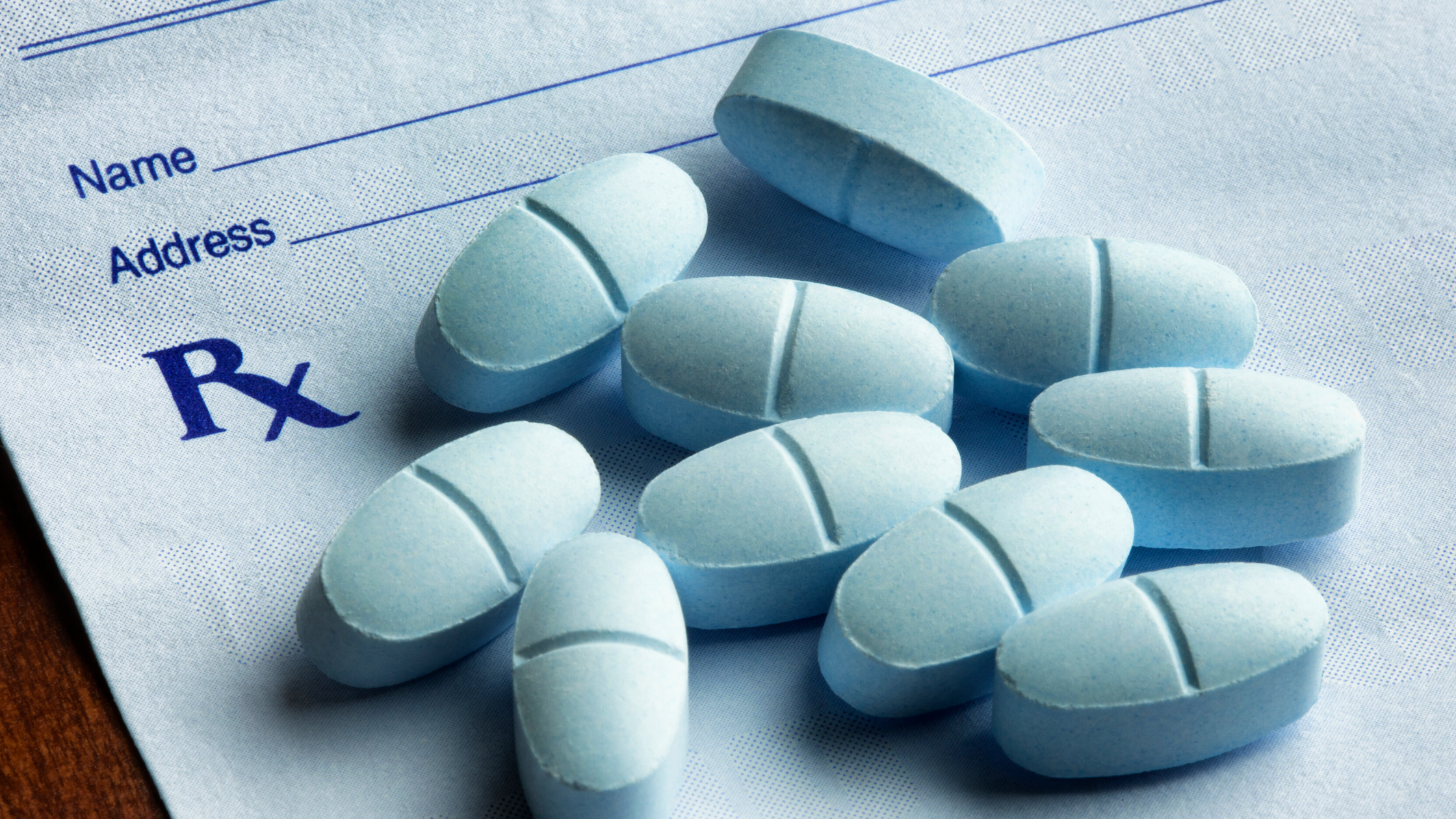
Opioid use disorder (OUD) is a pattern of use that includes the inability to reduce opioid use, decreased work/school performance, and increased time and effort spent obtaining opioids. OUD was first declared a public health crisis in 2017 and remains so today.
Statistics reveal that 15% of Americans filled at least one opioid prescription in 2018. The number of these deaths declined from 47,600 in 2017 down to 46,802 in 2018. That represents an average of 128 deaths each day in 2018. Given the still high number of opioid overdose-related deaths and the recent percentage of people still prescribed opioids, the need for opioid use treatment remains a priority for health care in the United States.
The problem with routinely prescribing opioid medications is that they can become addictive in as little as 4 to 8 weeks. The body quickly adapts to the presence of opioids and creates physical dependence on them. When this happens, stopping the opioid drug causes severe and unpleasant symptoms of pain, cravings, anxiety, sleeplessness, and a host of other complaints including gastrointestinal discomfort.
The clinical treatment protocol considered to be most effective is medication-assisted treatment (MAT). The programs were designed to meet the unique needs of patients diagnosed with OUD. They combined behavioral health services and medication in monthly bundles to allow for customization based on the patient and progress.
It is essential to report the opioid use disorder diagnosis correctly, to capture accurate data for health trends and statistical purposes. Health trends are used to evaluate health care needs, like additional treatment programs in areas that have reported increased statistics of OUD or meeting the definition of medical necessity for service coverage and reimbursement purposes. For example, some third-party payers may require specific condition codes related to opioid use, rather than status (history of) or withdrawal symptom codes.
Correct coding of bundled services for opioid treatment programs ensures success in reporting and reimbursement, and in doing so, supports the accessibility of these programs. Awareness of these codes and their correct use can start a new trend in healthcare that provides treatment to the underserved people with opioid use disorder. Upon completing Opioid Use Disorder Coding, you will be able to:
- Define opioid use disorder
- Describe the intent and use of medication-assisted treatments
- Summarize the treatment included in a MAT program
- Differentiate the service codes for a MAT program, versus office-based treatment
- Define the types of diagnosis codes used on claims for opioid use disorder
Ready to get started on these coding updates?